How did this extensive research start and what questions has it already answered? Ádám Dénes, head of the Momentum Laboratory of Neuroimmunology at the Institute of Experimental Medicine of the Hungarian Academy of Sciences (MTA KOKI), winner of an ERC Consolidator Grant last year, spent a long time at the University of Manchester, where he coordinated the research done by the research group studying the role of inflammation in stroke as part of the European Stroke Network, a programme of the European Union. Their research has found that inflammatory processes contribute to brain injury and diseases of the nervous system. Surprisingly, these processes often start in an organ other than the brain. Several common diseases (diabetes, arteriosclerosis, obesity, hypertonia, etc.) are also considered as chronic inflammatory conditions, which might affect cerebral inflammatory processes and progression of brain pathologies. Therefore, these widespread comorbidities and risk factors predispose patients to neurological diseases, including stroke, epilepsy, Alzheimer’s and Parkinson’s disease, what is more, to depression and certain mental disorders.
Cerebral inflammatory processes are predominantly regulated by the so-called microglial cells, which are specialised immunocompetent cells in the brain. Researchers found that the functioning of microglial cells has already changed in patients presenting with chronic systemic inflammation and several risk factors for stroke, but without any obvious signs of neurological disease: microglia showed increased activity. The increased incidence of stroke-events has also been observed during late autumn and early spring, which correspond to the “peak” season of respiratory infections, which also drive systemic inflammation. Through experimental studies it has also been demonstrated that inflammation not only precedes neurological conditions, but also actively contributes to the evolution of brain injury. At the same time, blockade of inflammatory processes reduces the extent of injury and improves functional outcome, suggesting that understanding these processes may have therapeutic benefits in the future.
What happens if the microglial cell is “switched off”, like a lamp? This is the question Ádám Dénes was trying to address after he returned to the MTA KOKI in Budapest, Hungary. Fortunately, he has managed to secure funding to proceed with his research. Over the past years, new sources of funding have been deployed to provide the financial basis for scientific research and to encourage researchers to stay in their home country, demonstrating a strong intention of the government. This intention is also reflected by the competitive calls announced under the Momentum Program, the National Brain Research Program or the NRDI Fund. The work of Ádám Dénes and his colleagues was also supported by the discovery of a drug family by one of the pharmaceutical companies cooperating with his research group, which blocks one of the molecular pathways required for the maintenance of the microglial cells in the brain, without having any serious effect on any other cells in the organism. This approach has made it possible to selectively eliminate glial cells from the brain without causing inflammation or apparent injury to other cell types. Once the administration of the substance was stopped, the microglial cells repopulated the brain, allowing researchers to recover microglia-associated functions as well.
When mice without microglial cells in the brain were exposed to an artificial stroke, brain injury increased by 60%. However, the return of microglial cells to the brain fully reversed this process, implying the important role of microglia in protecting neurons in the brain!
The next important stage of research was the establishment of collaboration between Ádám Dénes and the KOKI research group of Balázs Rózsa. They managed to combine for the first time the selective manipulation of microglial cells and advanced imaging technology, which enables the examination of cerebral inflammatory processes and the activity of damaged neurons after brain damage. They revealed by using high resolution two-photon microscopy how the functioning of the microglial cells is related to the activity of neurons. They found that microglial processes contact neurons in an activity-dependent manner. Selective elimination of microglia resulted in dysregulated neuronal activity in the injured brain and the rate of neural death increased. During their further studies Ádám Dénes and his research group also found that microglia sense and respond to neuronal activity changes under physiological conditions.
How do microglia contact neurons, and how does that interfere with the function of individual cells or complex neuronal networks? To this end, the research group of Dénes Ádám made use of super resolution microscopy, which is established at the MTA KOKI and had not been previously used to study the relationship between microglia and neurons. By applying this technology that allows the detection of individual molecules at 20 nanometres lateral resolution, they have identified specific receptors maintaining the “dialogue” between microglia and neurons.
Microglia-neuron contact sites have also been examined in 3D by applying a new and costly method, electron tomography, and importantly, not only in the brains of mice, but in post mortem human samples as well. It was shown that the key receptors accumulate at microglia-neuron communication hot spots, where specific “anchor” points are formed with several molecules playing a role in the transmission of signals between the two cell types – some of which have already been identified. This indicates the discovery of a new, so far unexplored microglia-neuron contact point in the brain. This anatomic phenomenon is present in most neurons and might be important in several diseases of the nervous system.
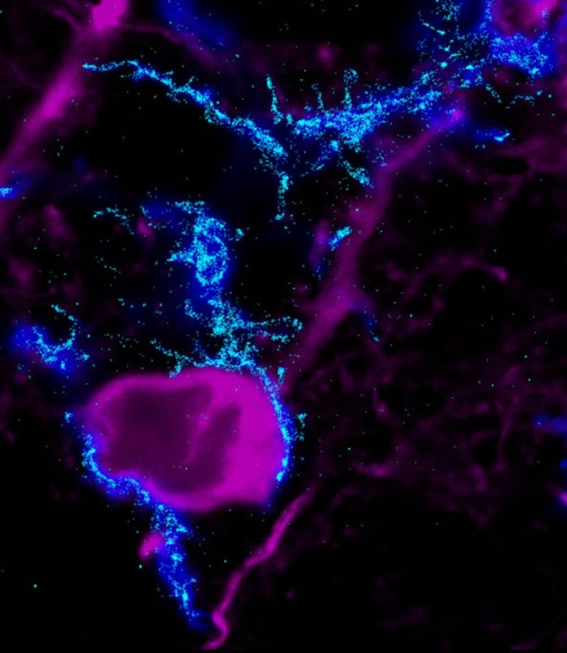 |
| Microglia-neuron interactions in the brain. The image made by the super resolution microscopy showing the distribution of microglial receptors that are essential for the formation of microglia-neuron contacts (by Barbara Orsolits) |
Microglia are not only responsible for the “dialogue” with neurons: they also eliminate improperly functioning synapses, and damaged or infected neurons and other cells from the brain. This “cleaning” must be extremely accurate and regulated, as an error made by the microglia would lead to a devastating outcome. The measurements and calculations made by the research group of Ádám Dénes show that our microglia cells could in theory “eat up” our brain in as few as 100 hours! How do the microglia decide what to eliminate and how is it possible that we may live up to 100 years? It has become clear that microglia recognise damaged cells partly with the help of receptors used to communicate with neurons. On the surface of injured neurons researchers also identified molecules which are involved in the phagocytosis of damaged cells. It means that several immune processes, however unexplored so far, might work in the nervous system. One key focus of research may be brain diseases to be be caused by the errors in the recognition and cleaning of damaged cells.
While there are numerous findings, many questions still remain unanswered. New knowledge and interconnected discoveries in this field of research will certainly lead to the development of medications with increased efficacy and new therapeutic implications to ease neurologocal diseases.
Work is undertaken within the framework of the National Brain Research Program. The research group of Ádám Dénes includes 1 senior researcher, 3 post-doctors, 4 PhD students, 1 technician and 3-4 university students participating in Students’ Scholarly Circle.
Find more information on previous research projects Ádám Dénes led or participated in, that were funded from the NRDI Fund.






